Our certified medical coders carefully review clinical notes and documentation to ensure accuracy, proper coding, and compliance with payer guidelines.



Pulsepapers is a trusted medical coding services provider with years of experience delivering accurate, compliant, and specialty-specific coding solutions for healthcare practices across the nation. Our certified medical coders support providers in improving documentation quality and reimbursement accuracy.
We specialize in ICD-10-CM, CPT, and HCPCS coding across multiple medical specialties. Every chart is carefully reviewed to ensure correct code assignment, reduced coding errors, and improved claim acceptance while meeting payer and regulatory requirements.
Patient data security is a top priority at Pulsepapers. Our medical coding processes strictly follow HIPAA compliance standards, ensuring complete confidentiality and protection of sensitive healthcare information.
By using advanced coding tools and ongoing coder training, we help providers stay aligned with evolving coding guidelines while reducing administrative workload and supporting accurate reimbursements.
With Pulsepapers Medical Coding services, providers gain a reliable partner committed to accuracy, compliance, and long-term financial success—allowing them to focus on delivering high-quality patient care.
Our medical coding services ensure accurate, compliant, and timely coding of clinical documentation, improving reimbursements and reducing claim denials.
Our certified medical coders carefully review clinical notes and documentation to ensure accuracy, proper coding, and compliance with payer guidelines.
Our certified medical coders carefully review clinical notes and documentation to ensure accuracy, proper coding, and compliance with payer guidelines.
We translate diagnoses, procedures, and treatments into standardized ICD-10-CM, CPT, and HCPCS codes for accurate insurance submissions and compliance.
We translate diagnoses, procedures, and treatments into standardized ICD-10-CM, CPT, and HCPCS codes for accurate insurance submissions and compliance.
We generate super bills and prepare claims with accurate coding, ensuring all services, payer responsibilities, and co-payments are correctly documented for faster
We generate super bills and prepare claims with accurate coding, ensuring all services, payer responsibilities, and co-payments are correctly documented for faster

Our specialized medical coding services ensure every diagnosis, procedure, and treatment is accurately translated into ICD-10, CPT, and HCPCS codes. By maintaining coding precision, we help healthcare providers reduce claim errors and avoid costly denials.
Using our in-house SmartCode system, all clinical documentation is thoroughly reviewed before submission. This technology and expert coder oversight help achieve high first-pass claim acceptance rates, accelerate reimbursements, and improve overall revenue integrity for medical practices.

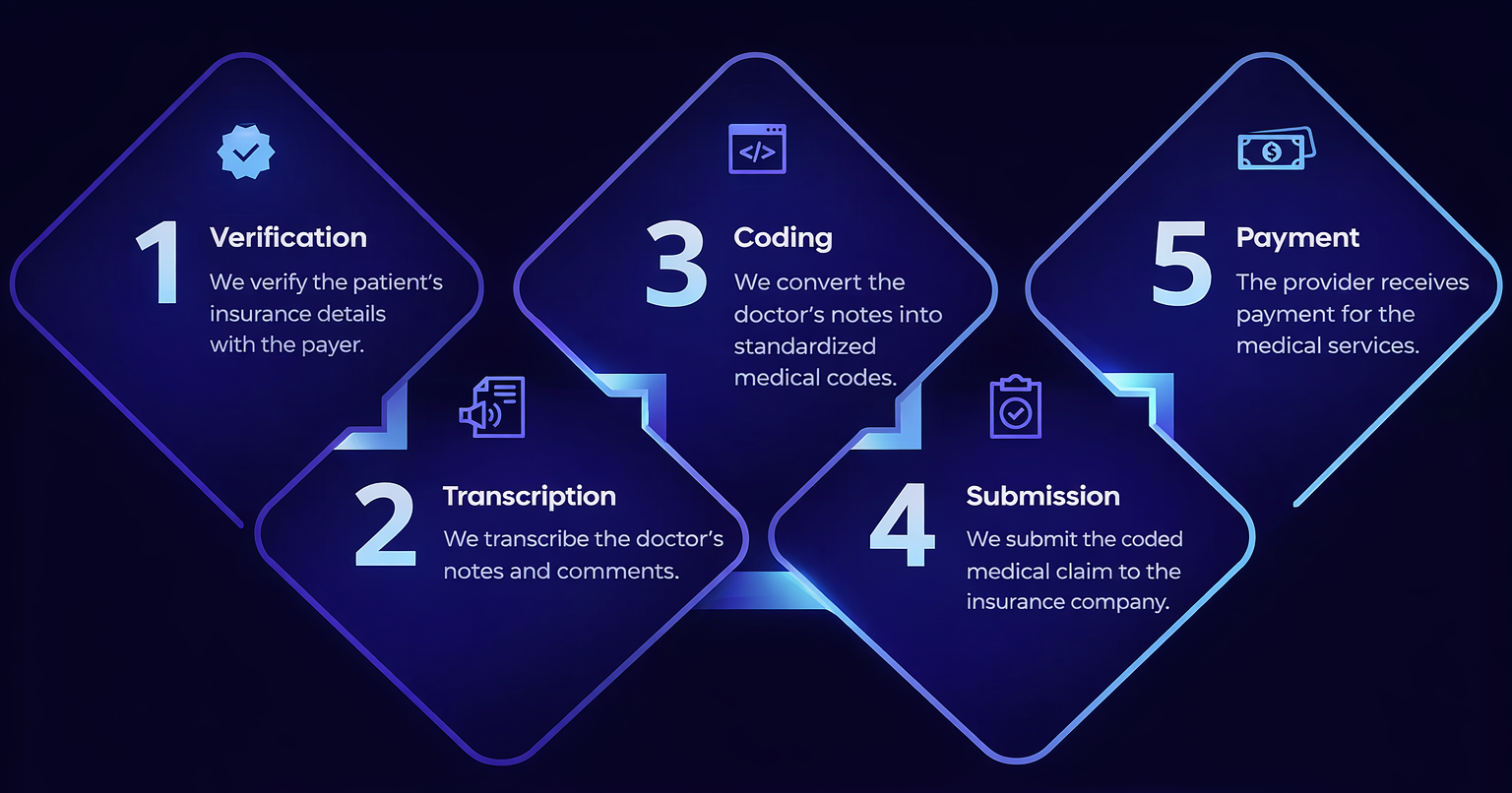

Our certified coders assign precise ICD-10, CPT, and HCPCS codes for every diagnosis and procedure, ensuring compliance with payer and regulatory standards.

All medical charts and notes are thoroughly reviewed to verify accuracy, improve documentation quality, and prevent coding errors before submission.

We prepare super-bills and ready-to-submit claims, capturing all patient charges, co-payments, and payer responsibilities for faster reimbursement.

Our team identifies reasons for claim denials, performs corrective actions, and implements preventive measures to minimize future denials.

All coding activities follow strict HIPAA standards, ensuring patient data is secure, confidential, and fully protected at every stage of the process.
Detailed coding reports provide insights into coding accuracy, reimbursement trends, and operational performance to support informed financial decisions.
Medical coding translates diagnoses, procedures, and treatments into standardized codes like ICD-10, CPT, and HCPCS. Accurate coding ensures proper reimbursement, compliance with regulations, and reduces claim denials.
Our certified coders use advanced tools and review clinical documentation thoroughly, verifying all codes and preventing errors before claims are submitted to payers.
We cover multiple specialties including cardiology, orthopedics, radiology, oncology, general practice, and more. Our coders are trained for specialty-specific coding requirements.
Denied claims are analyzed to identify root causes. Our team corrects coding errors, submits corrected claims, and implements preventive measures to minimize future denials.
Absolutely. All medical coding activities follow strict HIPAA compliance standards, ensuring patient information is secure, confidential, and protected at every step.
Accurate coding reduces claim rejections, speeds up reimbursements, and ensures your practice receives the maximum allowable revenue for every service rendered.